Achilles Tendonitis Rock Climbing
We’re here today to talk about your lower leg. My lower leg? In a climbing blog? Yes, those beautiful bulging rocks you call calves! Well, to be more specific, your Achilles tendon. Everyone “raves” about their shoulder injuries, but it’s time to pay some attention to your Achilles. Ever slip on a fresh new pair of climbing shoes and end up with weeks of “ankle pain in the back?” Bouldering in a climbing gym and notice a sharp pain at the back of your ankle pain every time you land? Or how about that pain down your ankle after a long approach or hanging belays? The irritation you may be feeling is coming from your Achilles tendon.
The Achilles tendon is the tendon from the gastrocnemius and soleus muscles. This tendon attaches directly to the heel of the foot. The tendon allows the gastroc-soleus complex to lift the heel off the ground, walk, and generate power during dynamic movements. Constant aggravation of the gastroc-soleus complex or the heel attachment can lead to inflammation at the Achilles tendon.
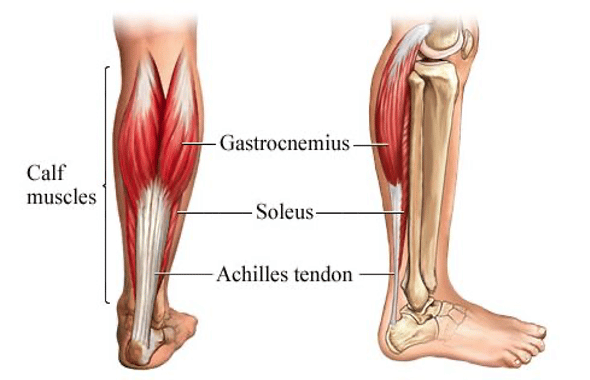
Achilles tendinopathy is less common with climbers but can impede climbing consistently. Considering that the lower leg is our workhorse and responsible for keeping us stable during climbs, managing Achilles tendinitis is essential. Proper care of this injury is the difference between sending climbs in a week to months of rest.
Signs and Symptoms
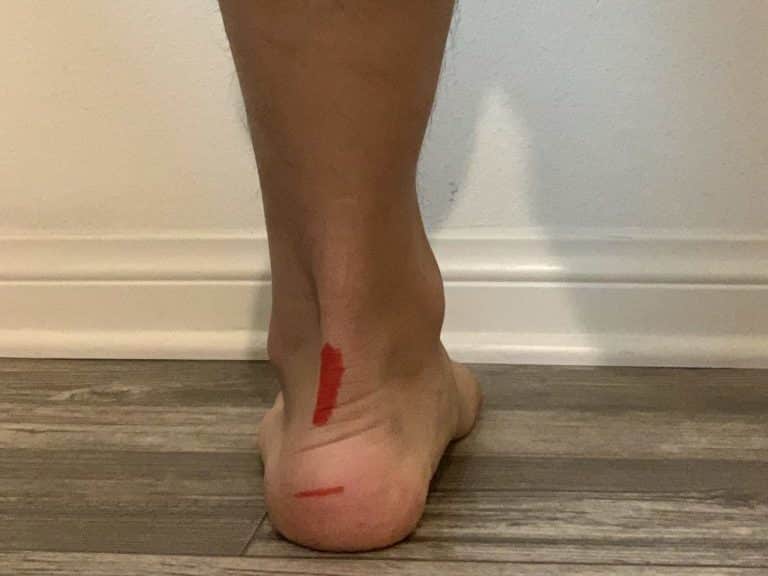
Common signs and symptoms are identifiable with self-assessment for Achilles tendinopathy. Aside from imaging techniques, there are ways to help determine if they possibly have Achilles tendinopathy. Achilles tendinopathy can be easily identified by its location. The two main areas of irritability are at the heel insertion or 2-6 cm above the insertion site. Signs and symptoms may include:
- Swelling
- Redness
- Thick tissue at the Achilles tendon which may resemble a bump
- Divot along the Achilles tendon
- Pain with palpation along Achilles tendon
- Pain with landing on feet at Achilles tendon
- Increased friction at the tendon site.
Climbers typically get Achilles tendinopathy from improper footwear, dynos, and poor landing techniques after climbing/bouldering. However, most climbers report pain in this area after long bouts of running, hiking, approaches, and descents. Symptoms that initially start from other activities can significantly impact a person’s ability to climb.
Assessment
Thompson Test
Before assessing tendinopathy, a possible rupture of the tendon must be ruled out. While standing, bend the knee and place the leg on a chair. While the leg is relaxed, reach back with the opposite hand and squeeze the calves. When performing the test, the ankle should move with the toes pointing. An absence of ankle movement when squeezing can mean a possible Achilles tendon rupture.
Palpation
Reach back and gently palpate along the tendon from the gastroc-soleus muscle belly to the calcaneus. Note where there are increased areas of discomfort during the palpation. A typical location of tendinopathy is 2-6 cm from the calcaneus. Be gentle with palpating the structure as the tendon can be sensitive to healthy individuals. Note the sensation on the opposite leg for direct comparison.
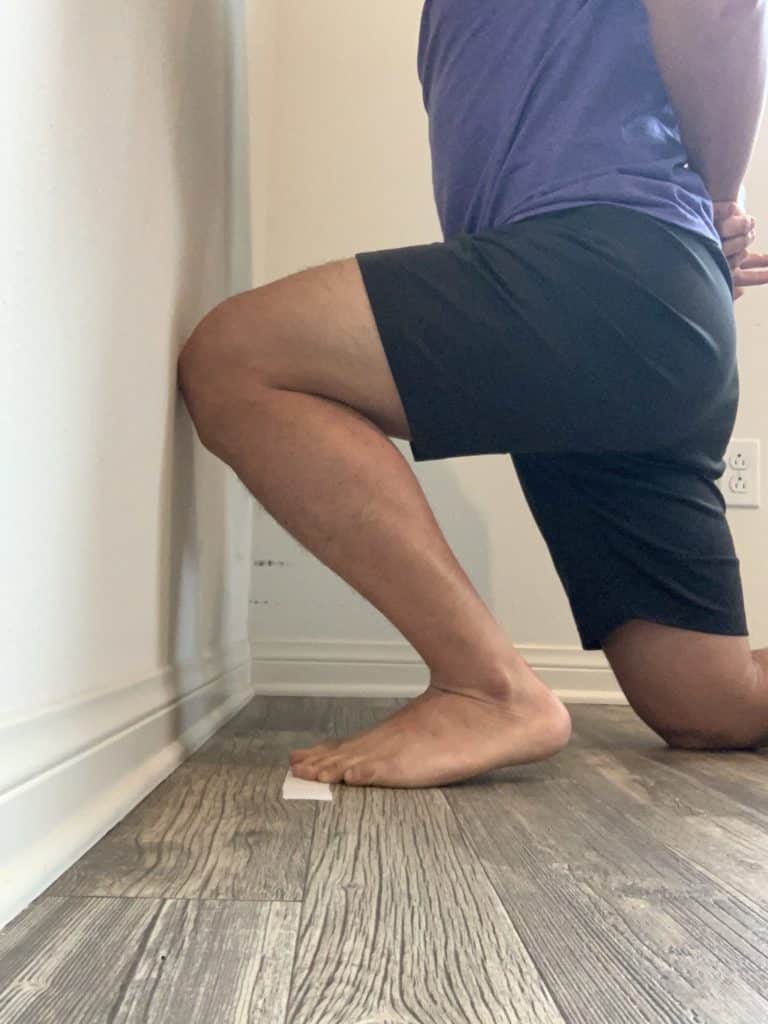
Ankle Mobility
Assume a half-kneeling position in front of a wall with both legs making a 90-degree angle. The front leg’s great big toe should be placed 10 cm from a wall. From here, attempt to have the front leg’s knee touch the wall with the front leg’s knee. Notice if the heel rises during the movement. The knee should be able to reach the wall with normal ankle mobility. The presence of heel rise can be caused by limited joint motion at the ankle or decreased muscle length.
Knee to Wall Correct

Knee to Wall Incorrect
Double leg squat/jump analysis
assess amount of pronation, dorsiflexion, and knee flexion during descending/landing phases
Place your body in front of a mirror and assume a squat position. Perform a squat and watch the knees and ankle during the movement. Notice if the knees cave inwards and the heel begins to rise. Improper movement may be the cause of increased stress at the Achilles tendon.
Next, perform a jump and land on both legs. Notice if the knee and ankle demonstrate similar patterns as the squat when landing.
Please note, positive findings from these assessments does not confirm a diagnosis of Achille’s tendinopathy.
The Rock Rehab Pyramid
The Rock Rehab Pyramid program is created by physical therapist and rock climber Dr. Jared Vagy and illustrated in his book Climb Injury-Free. The pyramid is broken down into four categories, progressing from the initial injury point to returning to climbing. Each section targets an essential aspect of recovery for the body. Below describes each type and example of treatment climbers can self-perform to return back to climbing.
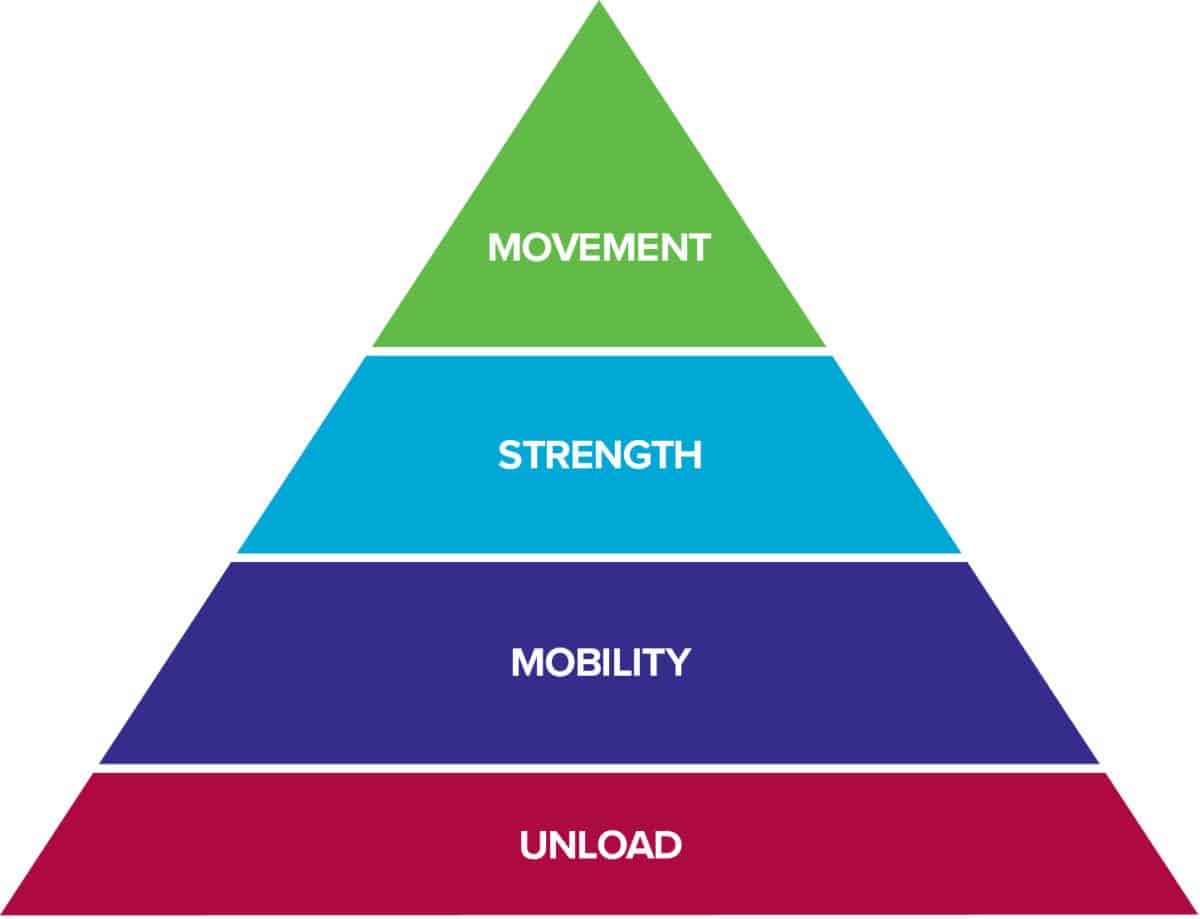
The bottom level of the pyramid aims to decrease Pain, Inflammation and Tissue Overload so that the tissues have the best healing environment. Often times, after an injury there is some sort of change in Mobility. After the tissues have calmed down from the previous level, this stage will look to reestablish normal, pain free range of motion. Once the injured area restores its mobility, it is time to increase the Strength of the surrounding muscles so that Movement in the following level can be coordinated and optimized. Click here to learn more about the rock rehab pyramid structure.
Unload
After the initial injury, the body will naturally go through a process of inflammation. Avoiding tissue aggravation is essential at this stage. Unloading the stress on the tendon will decrease further damage. It is recommended to avoid climbing at this time. Below are methods to minimize stress on the Achilles tendinopathy.
Heel Lift – As Needed
Wearing shoes/inserts that provide heel lift: A heel lift or shoe with a wedge can decrease tension on the tendon during everyday activities such as walking.

https://www.amazon.com
Taping – As Needed
Taping techniques for the gastroc-soleus muscles can provide support, reduce tension on the tendon, decrease inflammation, and allow ease of everyday activities during the healing process.
Mobility
Regaining appropriate mobility is necessary to avoid injury recurrence. Decreased ankle mobility is a common factor for Achilles tendinopathy. Mobility exercises should target the ankle joint and gastroc-soleus muscles. Appropriate movement at these areas will prevent excessive tension at the tendon.
Half kneeling dorsiflexion talocrural posterior glide w/ superband – assist with posterior glide of talocrural joint. 3×12
Assume a half-kneeling position with the affected leg in front. Wrap a superband around a supportive structure and place other end at the ankle of the front leg. Apply moderate tension in the resting position. Once appropriate tension is achieved, rock the body forward while maintaining the heel on the ground. Hold for 1 second before returning to original position.
Gastroc-soleus stretch against wall in split stance. 3×30 sec
Assume a split stance position and place hands on a wall. Make sure both knees are straight and heels touching the ground. Once the position is established, lean the body towards the wall. A stretch sensation of the gastrocnemius should be felt. To target the soleus, bend the back knee before leaning body forward. Remember to avoid painful stretching during this activity.
Gastroc-soleus stretch with heel off step 3×30 sec
Find an elevated platform (ex: staircase, step, box, etc.) to stand on. Make sure a supportive structure is nearby to hold onto. Place foot at edge of platform with the heel hanging off. Using the arms for support, drop the heel off the step as if you are falling backwards. Remember to avoid painful stretching during this activity.
Strength
Now that mobility is achieved, the next focus is strengthening the surrounding location. Strengthening the appropriate structures is necessary for shock absorption of the Achilles tendon. The exercises below are simple exercises that target possible deficiencies seen during the self-assessment. Climbing at this time can be resumed with limited repetition and appropriate rest.
Towel crunches for foot intrinsic 4×8
In a seated position and knees at 90 degrees, place a towel on the ground and place your foot on top. Flex the toes and create an arch, scrunching the towel. Hold for 1 second and relax the foot.
Gastroc-soleus heel raises 4×8
In a standing position, lift both heels off the ground and sustain the position for 2-3 seconds. Return heels to ground in a controlled rate before repeating activity. This exercise can be performed while maintaining holds overhead to simulate a climbing position.
Eccentric ankle plantarflexion 3×30
In a standing position and on an elevated platform, have both heels hanging off the platform. Using primarily the unaffected leg, rise up on the toes. At this position, stand on the affected leg and control the descent past the step for 5 seconds.
Double leg box jumps w/ soft landing 5×5
Although I don’t have a video of this exercise, it is very simple to do. Find an elevated platform roughly half the height of the lower leg. Assuming proper squat loading position, jump onto the box with a soft landing. Knees should be facing forward or outward with heels touching the platform when landing.
Movement
Movement exercises focus on ways to prevent future similar injuries while climbing. These movements should be implemented in your daily climbing regimen.
- When landing from bouldering, avoid having your feet and knee bend inwards during ground contact. Focus on bringing the hips back and avoid having the knees go excessively past the toes. This will decrease the amount of stress on the Achilles tendon after each jump.
- During heel hooks, engage the deep foot muscles to provide support when pushing on the hold. Similar to the towel crunch, create an arch in the foot once you are ready to move onto the next hold.
- Adjusting Hanging Belays – Create a makeshift belay seat to use during your climbs. Weighting the harness instead at the hip instead of feet decreases pressure at the Achilles tendon. Make sure to avoid long period of sitting for adequate blood flow at the thighs.

https://www.climbing.com/skills/how-to-maximize-comfort-at-hanging-belays/
The Research
- Cook JL, Khan KM, Purdam C. Achilles tendinopathy. Man Ther. 2002;7(3):121-130.
- Silbernagel KG, Crossley KM. A proposed return-to-sport program for patients with midportion achilles tendinopathy: Rationale and implementation. J Orthop Sports Phys Ther. 2015;45(11):876-886.
- Stevens M, Tan CW. Effectiveness of the alfredson protocol compared with a lower repetition volume protocol for midportion achilles tendinopathy: A randomized controlled trial. J Orthop Sports Phys Ther. 2014;44(2):59-67.
See a Medical Practitioner
To receive a proper evaluation and treatment seek a medical practitioner. Health care professionals such as physical therapists can assist with identifying the main deficits and appropriately treat injuries such as an Achilles tendon.
About the Author
My name is Eric Hwang and I am currently a student physical therapist at Mount Saint Mary’s University and a certified athletic trainer. I received my master’s degree in athletic training at West Virginia University and a bachelor’s degree in athletic training at Boston University. My previous experience includes treating and rehabbing collegiate athletes in the Division I,II,III levels. I love to go bouldering and have been slowly making the transition into top roping! You can contact me via e-mail, ehwang.fal@gmail.com or thru social media, IG: @cirehw.
- Disclaimer – The content here is designed for information & education purposes only and the content is not intended for medical advice.





Greetings from Greece! The article is a nice roundup. Unfortunately for me it does not mention insertional tendonitis, that is at the point of the horizontal mark (in your picture with the red marks) which is what bothers me for several months (still active and getting better).
My problem is that stretching aggravates the situation as does strengthening in dorsiflexion (most would agree).
Not quite easy to follow a strengthening protocol together with general exercise (running, general strength). As a (former) climber I have patience with tendons, but I would like advice on any negative signs (at the moment next day mild symptoms eg. senitive to touch or some irritation are common). I feel that I should press through these nuances, but I am afraid and act conservatively (age 52).
Climbers with insertional: seems like I disaster, it should be impossible to put on any climbing shoe, when irritated!
Towel crunch is interesting (I will try).
I am also thinking to try to stretch with toes bended upwards (et. the possition of the mobility test, eg. at a stair, with toes up and against the vertical part of the step). This would allow stretching with less dorsiflexion.
Best Regards and stay healthy!
Answered by Jared Vagy DPT:
Hey Costas,
Insertional tendinopathy is more difficult to treat and often doesn’t respond well to eccentrics. For example in the below study they had shown this:
Rufai A, Ralphs JR, Benjamin M. Structure and histopathology of the insertional region ofthe human Achilles tendon. J Orthop Res 1995;13(4):585 – 93.
However, clinically with insertional tendinopathies, I tend to put my emphasis further up the chain into the hip and further down into the foot. For example, focusing on hip flexor muscle length to achieve a trailing limb when walking and running and following that with glut max strength to absorb shock. Or focusing on frontal plane hip mechanics, i.e. gluteus medius – since the Achilles also inverts the rearfoot. Or addressing a stiff (or hypermobile) midfoot that may be leading to lack of shock absorption (or excessive prontation).
For footwear fit, there are a lot of tips and tricks for climbing shoes that involve different brands, models, lacing techniques and cuts.
There are a lot of directions to go. Best of luck!