Training for High Altitude Climbing

We approached the lower saddle of the Grand Teton as the sun slowly began to rise. There was a feeling of optimism due to our quick ascent of the hiking section on the Grand. We planned to climb the full Exum ridge parking lot to parking lot. With over 7,000 feet of ascent, we needed to move quickly. We had been hiking since midnight and neither me nor my partner had slept much, if at all. We hiked toward the first pitch and I began to feel nauseous and felt an aversion to eating or drinking anything. We made it to the base of the first pitch and I climbed with frozen hands, anchored, and belayed my partner. The climbing of the Exum ridge is easy to moderate as the crux pitches are rated 5.7. The difficulty was not the crux for me. The nausea increased as I sat on belay waiting for my partner to finish the next pitch. I felt dizzy, nauseous and had uncontrollable shivering. I met my partner at the end of the second pitch and confessed that I didn’t feel well enough to lead any more. Feeling nauseous and dizzy made me feel that leading could be dangerous for me, and I opted to follow for the rest of the climb. We made it up the last pitch of the lower Exum and bailed due to my condition. Once we made it back to the lower saddle my nausea and dizziness decreased, and my appetite returned.
What happened to me? I had climbed the Grand Teton before with minimal issues but this year my condition on the mountain stopped us from summitting. I talked to a mentor who had been a Teton ranger and he told me that mountain sickness can happen to anyone, no matter how often they climb. As I researched acute mountain sickness, I noted that I was experiencing many of the common symptoms. I have since wondered what could improve future ascents and possibly prevent any mountain sickness. It is common, for us as climbers, to want to climb high mountains and it is not always feasible to spend multiple days on the mountain acclimating. This article is for the weekend warrior who wants to climb in the mountains and prevent mountain sickness.
Signs and Symptoms
The disease of ascending into the mountains too quickly is known as high altitude illness (HAI). HAI includes acute mountain sickness (AMS), high-altitude cerebral edema (HACE) and high-altitude pulmonary edema (HAPE). HAI is caused by having less oxygen available in the air and therefore, in the blood. Typically, HAI onsets at 8,000 feet (2,500 meters) but some people may have symptoms from 5000-7000 feet (1500-2100 meters).1
AMS is the most common altitude disease that affects 40-50 percent of people who live at a low altitude and sleep above 10,000 feet. AMS symptoms include headache, feeling tired, lightheadedness or dizziness, lack of appetite, difficulty staying asleep, nausea, and sometimes vomiting. AMS symptoms are usually worse after the first night sleeping at a high elevation and reduce within a day if you do not ascend to a higher altitude. HACE is a progressive form of AMS that includes capillaries leaking blood into the cerebrum, a part of the brain, that causes increased pressure and swelling in the brain. Symptoms of HACE can include severe exhaustion or weakness, drowsiness, confusion, irritability, difficulty walking straight, and symptoms similar to intoxication. HAPE is a potentially fatal condition where lung capillaries leak blood into the lungs and fluid accumulates. It is uncommon but can happen to people who rapidly ascend to 8200 feet (2500m). Symptoms of HAPE include cough often with pink and frothy saliva mixed with mucus, breathlessness with activity and at rest, and difficulty walking uphill. These symptoms usually begin 4-5 days at high altitude and symptoms of AMS may or may not precede HAPE.1
| High Altitude Illness | elevation of onset of illness | Signs and Symptoms |
|---|---|---|
| Acute Mountain Sickness | 5000-8000 feet (1500-2500M) | headache, feeling tired, lightheadedness or dizziness, lack of appetite, difficulty staying asleep, nausea, and sometimes vomiting. |
| High-Altitude Cerebral Edema | continuing higher or staying at elevation of onset of untreated AMS | severe exhaustion or weakness, drowsiness, confusion, irritability, difficulty walking straight, and symptoms similar to intoxication |
| High Altitude Pulmonary Edema | 8200 feet (2500m) | cough often with pink and frothy saliva mixed with mucus, breathlessness with activity and at rest, and difficulty walking uphill |
Table 1
Action to Take If Experiencing High Altitude Illness
The initial action to take when experiencing any HAI is to begin to descend. The indication to descend instead of continuing onward can be linked to what type of HAI you are experiencing. AMS may not indicate the necessity of descent, but HACE and HAPE can indicate the need to descend. If beginning to experience symptoms of AMS, it will be important to monitor symptoms to be aware of the progression to HACE or HAPE. If you begin to notice symptoms of AMS, it will be important to try and rest more often during the ascent to not continue until symptoms resolve. Some medications can help to subside the symptoms of AMS. Ibuprofen (Advil) and Aspirin can be taken to subside headache symptoms. These medications can be purchased over the counter and may be a good option to have in your backpack when going into high altitude. Ondansetron (Zofran) is a prescription medication that can subside nausea and vomiting. Acetazolamide is another prescription medication that can be taken to prevent AMS, but also to treat the symptoms. Dexamethasone can be taken to reduce AMS symptoms. If necessary, supplemental oxygen can be used to reduce symptoms. Seeing your medical provider prior to a high altitude ascent may be beneficial to discuss current health and any need of prescription medications. Symptoms of AMS should resolve within 24-48 hours and if symptoms worsen you should descend and/or seek help.
Physiology of High-Altitude Exposure
What happens to physiology when the saturation of oxygen decreases with high altitude? To explain some of the effects of hypoxia the oxyhemoglobin dissociation curve will be used.
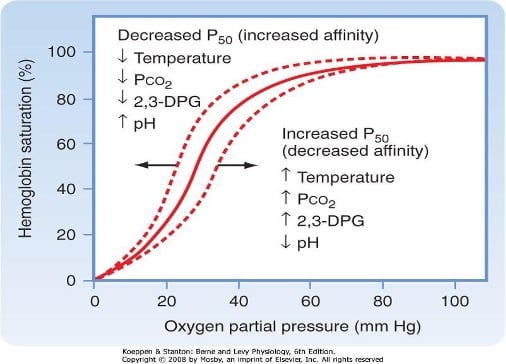
Scientists use this curve to show the attraction hemoglobin has for oxygen. Hemoglobin is a transport molecule that oxygen attaches to for transfer within the body to supply organs and tissues with oxygen. Oxygen can dissolve easily without hemoglobin and may not reach a target tissue without the transport of hemoglobin. With less attraction of hemoglobin to oxygen there is less available oxygen getting transported to our muscles and organs.2
As we ascend into higher elevation the partial pressure of oxygen decreases. This causes hypoxia in our body which means there is a lack of oxygen in our organs and tissues. Our first response to hypoxia is to breathe shallower and faster. Increased breathing rate causes the heart to beat faster and increase the pressure of oxygen. Faster shallow breathing also exhales increased amounts of CO2 which causes blood to become more alkaline which changes the balance of our blood. The body responds to the increase of pH by producing more bicarbonate, a base produced by the kidney, to balance the alkaline blood.3 Looking at the oxyhemoglobin dissociation curve, it can be seen how changes in altitude affects the acid base balance of the blood and influences P50. All these changes within our body can be handled through acclimatization.3 The body balances the acid base and normalizes hemoglobin’s attraction to oxygen. An increase of 2,3 DPG transports oxygen to tissues and moves the dissociation curve to the right.2 The issue is when a weekend warrior decides to make a push to the summit of a big mountain quickly. Not enough time is allowed for the body to acclimate and the climber becomes ill. Usually this will result in AMS which may or may not cause the climber to descend. Even if the illness is minimal, it still may affect how the climber feels when leading a difficult pitch.3
Can Physical Fitness Prevent High Altitude Illness?
As I began my study of high-altitude illness, I perused google searches of possible training programs and found a few blogs that supported aerobic training to improve breathing efficiency when ascending into high altitude.4,5 The American College of Sports Medicine (ACSM) defines aerobic training as any exercise that uses large muscle groups, can be maintained continuously, and is rhythmic in nature.6 Some of these activities are biking, hiking, running, or swimming. Aerobic activity is measured by the amount of oxygen consumed using a ventilatory measuring device (VO2). Exercise testing can be performed using graded with a cycle ergometer or treadmill to find an individual’s VO2max. Alternatively anaerobic activity is intense exercise of short duration independent of inhaled oxygen.6 While these blogs were well written and good advice was presented, none of these blogs cited sources or why the training suggested was science based.4,5 While learning from experience is the base of human knowledge, I felt that there should be some objective information available. The blogs I read discussed several activities but at the base of the advice was performing endurance activities for a higher VO2max. The theory was presented that a higher aerobic fitness improves breathing efficiency and prevent acute mountain sickness.4,5

Does Higher Aerobic Fitness Help Decrease Chances of High Altitude Illness?
A 2018 study investigated submaximal exercise testing at low altitude for prediction of high-altitude exercise performance. Forty participants performed a submaximal step test at low altitude (600m), 2-5 hours after reaching higher altitude (approximately 3500m) and again that afternoon. The step test exercise was performed in 2-minute bouts with 60 steps up and down a 24cm step. The following day all participants went on a 3–4-hour hike at high altitude with a pace that would be usually for regular guided tours. All participants were assessed for acute mountain sickness. Overall, 7 out of 31 participants developed AMS and had a maximal %HRmax below 86%. The conclusion of this study is that heart rate during submaximal fitness testing at low altitude can predict the onset of AMS at high altitude.7
Another study from 2018 studied if the 3-minute step test would predict the onset of AMS. This study had a larger sample size at 102 participants. The participants performed a three-minute step test at 250m and then again at 3,100m. The step test was performed as participants stepped up and down a 35 cm step at a rate of 24 steps per minute for three minutes. The participants were taken by bus from an altitude of 250m to 3,100m with a quick ascent of four hours. The participants were checked for AMS at 10 checkpoints along the ascent. A night was spent at elevation and participants were assessed for AMS the following day. The only difference seen between participants who had AMS and who didn’t was heart rate.8
So, we have two articles that indicate that submaximal testing as a predictor of AMS is linked to heart rate. It would be an easy hypothesis to say that climbers should perform endurance-based activities as one of the by-products of endurance training is lower heart rate.9 This lines up with the studies available and would give good backing to performing endurance training for AMS prevention. The issue with accepting this hypothesis is that there could be weaknesses in these studies. The studies were taken with a general population in mind and compared results with untrained individuals and did not specify if the individuals had any previous training.
A study from 2019 investigated the risk of AMS in endurance athletes. This study compared endurance trained athletes to an untrained control group. The participants performed VO2max testing at 424m. They were then transported to 750m and spent one night. On the next morning they were transported by train to 3450m. Examination of participants was performed at 3, 8, 24, 34, and 48 hours after arrival. What the researchers found during the testing is that endurance trained individuals have higher parasympathetic activity at low and high altitude. Parasympathetic and sympathetic activity is part of our autonomic system that keeps our body in a state of homeostasis. Sympathetic activity initiates our “flight or fight” centers and is activated when the body is in a state of distress. Parasympathetic activity, on the other hand, initiates the “rest and digest” systems of our body. The endurance trained athletes showed a higher rate of AMS during the first 24 hours of high-altitude exposure. The research found that the greatest difference between groups was increased parasympathetic activity and resting metabolic rate in the endurance trained participants.10 A quote from this article states “It is well established that the autonomous nervous system plays a major role for adaption to hypoxia by shifting the autonomic control towards sympathetic dominance to maintain oxygen transport to the tissue. Individuals who present with a higher parasympathetic activity, as ET (endurance training), may be prone to a delayed adjustment of sympathovagal balance in resting conditions at HA with increasing risk for early AMS.” 10 This means that by having a higher parasympathetic activity of endurance trained athletes a delay in adjustment at high altitude may occur.
Should we perform aerobic exercise for high altitude endeavors? The likely answer is that more research needs to be conducted to know the best way to train for high altitude environments. The literature reviewed in this article suggests that aerobic training alone should not be performed. Anaerobic strength does not decrease with high altitude, but aerobic strength decreases as much as 15%-20%.3 If you are living at a low altitude and you only plan on distance running or hiking to prepare to be ready for altitude conditions, it may not be as helpful as multiple training stimuli. When training for high altitude a mixture of strength, interval and endurance training may be important to perform compared to endurance and climbing training alone.
Sample Interval Training
The sample exercises I would recommend are full body exercises that can work well into an interval circuit. Interval training has the possibility of training both anaerobic function as well as a cardiopulmonary response. Using full body exercises can utilize muscles we need to strengthen as climbers. Interval training or High Intensity Interval Training (HIIT) is described by the ACSM as “repeated bouts of high intensity effort followed by varied recovery times.”11 HIIT exercise is performed with interval bouts followed by bouts of rest and should be performed with the heart rate at 80-95% of your maximum heart rate.11 Heart rate max can be calculated by performing the following equation:
Max heart rate=207-(0.7xAge)12
For HIIT protocol the 4×4 method is most generally used.13 The 4 x 4 method relates that 4 minutes of exercise are spent performing at 80-95% of HR max intensity and then 3 minutes at 70% HR max for 4 sets.14 To monitor heart rate there are many watches that can be purchased for this purpose. A cheaper option is to use a pulse oximeter that can be purchased at most drug stores. If no equipment is available, you can feel the side of your neck on the left or right side to feel the carotid artery. After finding a pulse on your neck you can use a timer and count the beats for 30 seconds. Then multiply that number by 2 and it will be your beats per minute. Practice a few times and then try to track the heart rate during the rest period of the exercise prescription. Exercises can be progressed by increasing weight, increasing sets, and increasing time of sets. Some possible examples for full body exercises that can be applied to a HIIT workout are below. The videos for these exercises were performed slower than high intensity to show proper form through the movements.
Kettlebell Squat to Swing.
Begin in a squatted position and swing the kettlebell up while extending the legs using momentum to swing up the kettle bell. This exercise strengthens the knee extensors, the ankle plantar flexors, the wrist flexors and the shoulder flexors.
Dumbbell Pushup to Row
Begin in a plank position holding on to dumbbell handles. Pay attention to the level of back and hips and attempt to keep a straight neutral position. Perform a push up by lowering down to dumbbells and press up back into starting position. Be sure to keep elbow position within a 45 degree angle from the shoulders. Once back to starting position one arm will pull the dumbbell up to the side keeping the back and hips level as possible. Pull the elbow back and keep the arm close to the side. perform push up again and repeat for the other side. This exercise is working the upper extremity pushing and pulling muscles as well as trunk musculature. Exercise as seen performed by Renan Ozturk in the film Meru.
Reverse Lunge with Kettlebell Hold
Begin by holding the kettlebell next to the body with arms at the side. Step back with one leg while keeping the trunk as straight as possible. Lower back leg knee toward the floor. Push up with forward leg and bring back leg back to starting position. Repeat on the opposite side. This exercise will work the ankle dorsiflexors, hip extensors and knee extensors. Isometrically (contraction without movement), this exercise will work the wrist and elbow flexors and shoulder stabilizers.
Plank Kettlebell Pull Throughs
Place the kettlebell on one side of the exercise area and then start in a plank position on hands with elbows extended. Attempt to keep hips and back in a straight neutral position during exercise. reach with the opposite hand to the kettlebell allowing minimal rotation of the spine and lift the kettlebell to the outside of the plank stance. reverse the activity with the other hand. This exercise works the core stabilizers and rotators, shoulder extensors, elbow flexors and wrist flexors.
Sample Exercise Prescription
- Following a warm up then begin with a 4 minute high intensity segment (80-95% Max HR).
High intensity segment
- Minute 1 Kettlebell Squat to Swing
- Minute 2 Dumbbell Pushup to Row
- Minute 3 Reverse Lunge with Kettlebell hold
- Minute 4 Plank Kettlebell Pull Through
Low intensity segment
- Perform 3 minutes of lower intensity exercise such as jogging, cycling or rowing (70% HR Max).
- Repeat exercise prescription for 4 sets.
- Beginners- start at 80% HR max and train up to 95%. If one set is very difficult at 80% then start with one or two sets and work up to four. This training can be included into climbing training. For a distance trained runner who is an alpine climber it may be beneficial to perform interval training once to twice a week in place of a distance run.
Conclusions
This article discussed the types of high altitude illness, associated symptoms and physiologic response. It is the intent of this article to review a portion of the literature that shows a response to exercise performance and high altitude. It was found that a better submaximal VO2 test showed decreased incidence of HAI. The literature also showed that endurance trained athletes had a higher incidence of HAI in the first 24 hours of high altitude exposure. It is the recommendation that when training for high altitude climbing a mix of strength training, interval training and endurance training should be considered compared to only endurance and climbing training. An interval training protocol with suggested exercises was given to facilitate different training stimulus then endurance training alone. Future research will be beneficial to better understand the cardiopulmonary response to high altitude with different training stimulus.
See a Doctor of Physical Therapy
If you have experienced a HAI and have continued symptoms, consider seeing a Doctor of Physical Therapy as part of your health care team. Physical Therapists obtain knowledge during university studies that include cardiorespiratory and cardiopulmonary understanding. Physical Therapists are often thought of for musculoskeletal injuries, but many people could benefit from seeing a Physical Therapist. Other conditions such as long COVID-19, pneumonia and heart failure could benefit from working with a Physical Therapist.
Author Bio

Ben Moore is a second year Doctor of Physical Therapy student at Idaho State University. He has been climbing since 2016 and started climbing during his undergraduate studies at Idaho State University. He enjoys applying physical therapy components to rock climbing and vice versa. He now lives in Pocatello, Idaho and can be found on Facebook: Benjamin Moore and Instagram: @bemoore808
References:
- Gallagher SA, Ganetsky DF. Patient education: High-altitude illness (including mountain sickness) (Beyond the Basics). UpToDate. https://www.uptodate.com/contents/high-altitude-illness-including-mountain-sickness-beyond-the-basics#H1. Published May 18, 2022. Accessed January 24, 2023.
- Winslow RM. The role of hemoglobin oxygen affinity in oxygen transport at high altitude. Respiratory Physiology & Neurobiology. 2007;158(2-3):121-127. doi:10.1016/j.resp.2007.03.011
- DeWeber K, Scorza K. Return to activity at altitude after high-altitude illness. Sports Health: A Multidisciplinary Approach. 2010;2(4):291-300. doi:10.1177/1941738110373065
- How to train for mountaineering: Rei Co-op. REI. https://www.rei.com/learn/expert-advice/mountaineering-how-to-cross-train.html. Accessed January 24, 2023.
- Parnell D. How to train for high altitude hiking at sea level. Trail and Summit. https://trailandsummit.com/how-to-train-for-high-altitude-hiking-at-sea-level/. Published June 30, 2022. Accessed January 25, 2023.
- Patel H, Alkhawam H, Madanieh R, Shah N, Kosmas CE, Vittorio TJ. Aerobic vs anaerobic exercise training effects on the cardiovascular system. World Journal of Cardiology. 2017;9(2):134. doi:10.4330/wjc.v9.i2.134
- Burtscher M, Philadelphy M, Gatterer H, Burtscher J, Likar R. Submaximal exercise testing at low altitude for prediction of exercise tolerance at high altitude. Journal of Travel Medicine. 2018;25(1):1-4. doi:10.1093/jtm/tay011
- Chiu T-F, Chen LL-C, Su D-H, et al. Rhodiola crenulata extract for prevention of acute mountain sickness: A randomized, double-blind, placebo-controlled, crossover trial. BMC Complementary and Alternative Medicine. 2013;13(1). doi:10.1186/1472-6882-13-298
- Carter JB, Banister EW, Blaber AP. Effect of endurance exercise on autonomic control of heart rate. Sports Medicine. 2003;33(1):33-46. doi:10.2165/00007256-200333010-00003
- SAREBAN MAHDI, SCHIEFER LISAM, MACHOLZ FRANZISKA, et al. Endurance athletes are at increased risk for early acute mountain sickness at 3450 m. Medicine & Science in Sports & Exercise. 2019;52(5):1109-1115. doi:10.1249/mss.0000000000002232
- Riebe D, Ehrman JK, Liguori G, Magal M. 5 . In: ACSMS Guidelines for Exercise Testing and Prescription. Philadelphia, PA: Lippincott Williams & Wilkins; 2019:149.
- High-intensity interval training – american college of sports medicine. https://www.acsm.org/docs/default-source/files-for-resource-library/high-intensity-interval-training.pdf?sfvrsn=b0f72be6_2. Accessed January 25, 2023.
- Ito S. High-intensity interval training for health benefits and care of cardiac diseases – the key to an efficient exercise protocol. World Journal of Cardiology. 2019;11(7):171-188. doi:10.4330/wjc.v11.i7.171
- Acala JJ, Roche-Willis D, Astorino TA. Characterizing the heart rate response to the 4 × 4 interval exercise protocol. International Journal of Environmental Research and Public Health. 2020;17(14):5103. doi:10.3390/ijerph17145103
- Figure 1 From: Oxygen hemoglobin dissociation curve curva de disociacion … GrepMed. https://www.grepmed.com/images/6540/cardiology. Published December 5, 2019. Accessed January 25, 2023.
- Disclaimer – The content here is designed for information & education purposes only and the content is not intended for medical advice.




