From a Drop Knee To an ACL Injury! Returning To Climbing Post ACL Rupture
It’s your flash attempt on the highly anticipated V5 vert on the new set, you’ve waited patiently cheering your friends in their attempts, and it was finally your chance to send it. ALLEZ! You are pushing your grade as beads of sweat collect on your fingertips. As you fight to the crux, you pull hard on the left while pivoting your right toe in that fresh pair of drago LV’s. Twisting your hip inwards, tension builds on the outer side of your knee. Just a few more inches and you can reach the to-POP!!! You fall what you perceive to be lightyears to the ground, immediately surrounded by a thick mist of moon dust. You try to get up, but your knee buckles and terror and pain cloud your thoughts…
Background & Causes
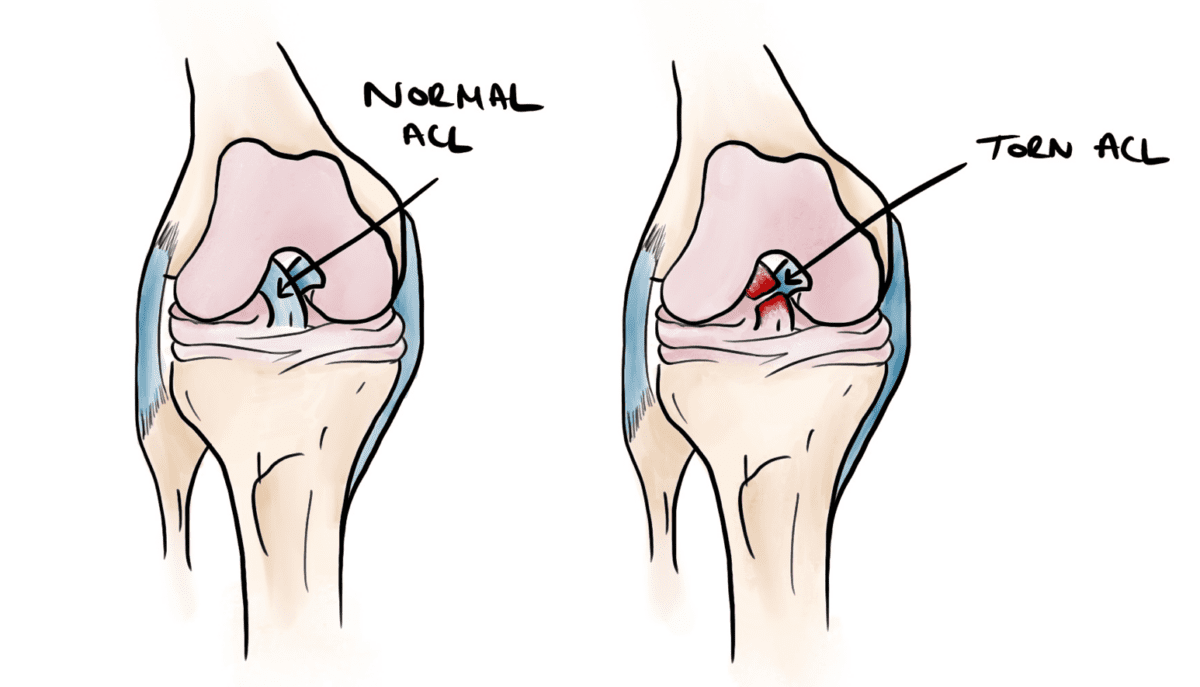
The knee joint is a common site of injury in climbing, injury can often occur due to trauma, or repetitive activities. There are many structures help the knee to both bend and straighten, as well as stabilize our body when we are standing or moving around, one of which being the Anterior Cruciate Ligament (ACL) deep within the knee joint, a structure involved in bridging our thigh and shin bones and the knee stability for ease of movement.
Drop knees, high step ups, heel hooks and ground falls are all common techniques that climbers employ which can put strain on the structures of the knee, possibly resulting in ruptures of the ACL ligament (11).
Risk factors
There are various factors that increase your chances of having an ACL injury – including the frequency and intensity at which we climb.
Other risk factors include:
- Being female already puts you at an increased risk- I hate to say it ladies! (1)
- Previous injury to the knee (1)
- Hypermobility- due to ligament laxity (1)
- High BMI (body max index) (2)
- Age (as we age the integrity of our joints, and the amount of muscle mass reduces) (13)
Signs and Symptoms
Did you feel an uncomfortable shifting sensation at your knee or hear an audible POP mid climb? These are often signs of an ACL tear. You might now be feeling pain at the knee while standing or walking.
Here are some other things to look out for after injury:
- Pain on the outside or the back of knee
- Swelling within the first few hours
- Difficulty with normal range of movement
- Feelings of instability or giving way
- Pain when weight bearing
If you feel any combination of these symptoms, it is important that you stop climbing and see a professional for medical advice.
See a Doctor of Physical Therapy
A physiotherapist can conduct various tests to confirm the diagnosis and or rule out injuries to other structures. Depending on their clinical findings, they can refer you onto the medical professional for imagining or a consultation regarding surgical management, depending on the severity of your injury, and provide you with a series of appointments alongside a treatment plan for managing the injury conservatively and getting back to doing what you love.
Your physiotherapist will have a plethora of functional tests at their disposal to determine your progress with treatment and readiness, so trust them to work with you and your goals!
Assessment
There are 3 main diagnostic tests Physiotherapists use to determine ACL ruptures:
- Lachmans test
- Anterior draw test
- Pivot shift test
Stages of rehabilitation:
Now onto the hard work. It is important to regain early movement after your injury and activate the quadriceps muscles in the thigh on the front of your leg. ACL injuries can make it difficult to straighten your knee, so it is crucial to work on mobilizing exercises to regain full extension within 2 weeks after injury.
The unaffected side can also often develop compensatory movement mechanics, which can influence the rate of incidence of reinjury, therefore engaging both limbs in rehabilitation is essential.
Stage 1: Unloading immediately post injury (0-2 weeks)
The protocol for pain management and deloading after injury involves icing, compressing, elevating and taking NSAID’s for the inflammation. At this phase, we will work on increasing range and initiating isometric muscle contraction with the following exercises:
- Lying heel slides (flexion) actively or use good leg passively
- Lying knee towel push down’s (iso extension)
- Quads mid-range isometric (towel under knee)
Stage 2: Strength and balance (once regaining full ROM) 3-5 weeks
At this stage we will work on building the strength of the large surrounding muscles of the knee joint such as the quadriceps on the front of the thigh and the hamstrings on the back side. Equally, we will work on balance to increase your awareness of your body in space, what we call proprioception.
- Bridges
- Standing leg curl
- Lying clams
- Partial squat/ wall sits
- Single leg standing- uneven surface (balance)
Stage 3: Progressed strength and balance exercises (6-8 weeks)
At this stage we will be advancing the strength and balance exercises to include weights or other increases in load and demand on the muscles. We will also include multiplane movement to begin to train the knee to experience loads and movement from other directions, what we call planes of movement.
- Bridges on stab ball
- Squats
- Step ups
- Lateral hop (multiplane with band)
- Lunges
Stage 4: Plyometrics (12 weeks+)
At this later stage of rehab, we will introduce speed and agility drills to increase muscular power with speed and velocity. This helps the knee to be able to withstand jumping and rebounding exercises and get you that much closer to returning to the sport you love. It is important to wait to begin plyometrics until your knee is stable, strong, and your are cleared by your surgeon and physical therapist. Some athletes begin at 8 weeks, some wait until 12, some wait until much later. It all depends on the athlete.
- Double leg jump> single leg jump
- DL Drop downs from height> SL drop down from height (16)
- Lateral step up/ jump
- Figure 8/ T Test agility drills (gait retraining with directional forces)
- Continued progressive strengthening exercises- NORDIC CURLS
Returning to sport
It can take around 9-12 months for a full recovery with extensive rehab with drive to get back into your sport. But we must bear in mind that the rate of recovery can be influenced by various factors including hesitancy, lack of confidence, and fear of reinjury. Don’t underestimate the psychological influence, lack of confidence of fear and pain avoidance tactics can result in abnormal movement patterns too.
The incidence of re-injury in the first two years following reconstruction is also estimated to be 6 times greater than those who didn’t suffer ACL injury, This incidence too is much higher in female athletes than males! Therefore, it’s important to follow a personalized progressive rehab program to continue to build on your strength and balance.
You must pace yourself for your return! Start with climbing lower grades. As always, practice caution by warming up properly, climbing within your abilities, taking appropriate rests and drinking plenty of water. Finally, that important precaution we always neglect to take… climb down where available!
Bulletproofing for the future
When returning to sport, it is important to consider that reinjury remains a risk factor.
Deficits in the quadriceps muscles in the front of our thighs is common, resulting in instability.
Unfortunately a history of injury puts you at an increased likelihood of having another. The following Four deficits have been considered to be risk factors for second ACL injury:
- Hip rotational deficits.
- Excessive frontal-plane knee mechanics (only training knee muscles uni directionally)
- Knee flexor deficits.
- Poor postural control (Big stabilizing muscles + core control)
Continuing with strength and balance training: It’s important to continue to increase muscle strength to support the structure of the knee, improve balance for increasing proprioception and to ensure that muscles tendons and joints can adapt to quick or unexpected movements.
In terms of minimizing your risk of reinjury, or further injury; Don’t neglect your warm ups. This is a vital part to ready the body for increased movement. Alongside this, It is equally important to practice mobility, falling safely as well as being able to recognize signs of injury for the future.
Your Information
I’m Grace Kelly West, a recent graduate from the University of East London. I live in northwest London in the UK. Being an avid climber of the past 3 years, both bouldering and lead, I particularly love to climb outdoors- though sadly this can be difficult with the English weather.
I embarked on my journey to train to be a physiotherapist after experiencing stubborn knee pain, and having sub-optimal rehab, so I decided I wanted to become the expert. I currently work for the London Climbing Centers group, the largest climbing institution across London, setting an exemplary standard for climbing across the country, with 8 centers just within London where I get to express my love for climbing and people on a regular basis.
Instagram: @gracekellywest

The Research
- Acevedo, R.J., Rivera-Vega, A., Miranda, G. and Micheo, W. (2014). Anterior Cruciate Ligament Injury. Current Sports Medicine Reports, 13(3), pp.186–191. doi:https://doi.org/10.1249/jsr.0000000000000053.
- Alsayed, H., Alkhateeb, M., Aldossary, A., Houbani, K., Aljamaan, Y., Alrashidi, Y., Al Munawara, M., Arabia, S., Madinah, A. and Munawara, A. (2023). Risk of anterior cruciate ligament injury in populations with elevated body mass index, [online] 20(1). doi:https://doi.org/10.17392/1517-22.
- Ayeni, O.R., Chahal, M., Tran, M.N. and Sprague, S. (2012). Pivot shift as an outcome measure for ACL reconstruction: a systematic review. Knee surgery, sports traumatology, arthroscopy: official journal of the ESSKA, [online] 20(4), pp.767–777. doi:https://doi.org/10.1007/s00167-011-1860-y.
- Buckthorpe, M. and Della Villa, F. (2021). Recommendations for Plyometric Training after ACL Reconstruction – a Clinical Commentary. International Journal of Sports Physical Therapy, [online] 16(3). doi:https://doi.org/10.26603/001c.23549.
- Casteleyn, P. and Handelberg, F. (1996). NON-OPERATIVE MANAGEMENT OF ANTERIOR CRUCIATE LIGAMENT INJURIES IN THE GENERAL POPULATION. 78-B(3), pp.446–451. doi:https://doi.org/10.1302/0301-620x.78b3.0780446.
- Coffey, R. and Bordoni, B. (2022). Lachman Test. [online] PubMed. Available at: https://www.ncbi.nlm.nih.gov/books/NBK554415/#:~:text=The%20Lachman%20test%20is%20a.
- Cole, K.P., Uhl, R.L. and Rosenbaum, A.J. (2020). Comprehensive Review of Rock Climbing Injuries. Journal of the American Academy of Orthopaedic Surgeons, 28(12), pp.e501–e509. doi:https://doi.org/10.5435/jaaos-d-19-00575.
- Joreitz, R., Lynch, A., Rabuck, S., Lynch, B., Davin, S. and Irrgang, J. (2016). PATIENT-SPECIFIC AND SURGERY-SPECIFIC FACTORS THAT AFFECT RETURN TO SPORT AFTER ACL RECONSTRUCTION. International Journal of Sports Physical Therapy, [online] 11(2), pp.264–278. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4827369/.
- LaBella, C.R., Hennrikus, W. and Hewett, T.E. (2014). Anterior Cruciate Ligament Injuries: Diagnosis, Treatment, and Prevention. PEDIATRICS, [online] 133(5), pp.e1437–e1450. doi:https://doi.org/10.1542/peds.2014-0623.
- Lutter, C., Tischer, T., Cooper, C., Frank, L., Hotfiel, T., Lenz, R. and Schöffl, V. (2020). Mechanisms of Acute Knee Injuries in Bouldering and Rock Climbing Athletes. The American Journal of Sports Medicine, 48(3), pp.730–738. doi:https://doi.org/10.1177/0363546519899931.
- Markéta Kovářová, Petr Pyszko and Kateřina Kikalová (2024). Analyzing Injury Patterns in Climbing: A Comprehensive Study of Risk Factors. Sports, 12(2), pp.61–61. doi:https://doi.org/10.3390/sports12020061.
- Paterno, M.V., Kiefer, A.W., Bonnette, S., Riley, M.A., Schmitt, L.C., Ford, K.R., Myer, G.D., Shockley, K. and Hewett, T.E. (2015). Prospectively identified deficits in sagittal plane hip–ankle coordination in female athletes who sustain a second anterior cruciate ligament injury after anterior cruciate ligament reconstruction and return to sport. Clinical Biomechanics, 30(10), pp.1094–1101. doi:https://doi.org/10.1016/j.clinbiomech.2015.08.019.
- Salzler, M.J., Chang, J. and Richmond, J. (2018). Management of Anterior Cruciate Ligament Injuries in Adults Aged >40 Years. Journal of the American Academy of Orthopaedic Surgeons, 26(16), pp.553–561. doi:https://doi.org/10.5435/jaaos-d-16-00730.
- Schöffl, V., Morrison, A., Schwarz, U., Schöffl, I. and Küpper, T. (2010). Evaluation of Injury and Fatality Risk in Rock and Ice Climbing. Sports Medicine, 40(8), pp.657–679. doi:https://doi.org/10.2165/11533690-000000000-00000.
- van Grinsven, S., van Cingel, R.E.H., Holla, C.J.M. and van Loon, C.J.M. (2010). Evidence-based rehabilitation following anterior cruciate ligament reconstruction. Knee Surgery, Sports Traumatology, Arthroscopy, 18(8), pp.1128–1144. doi:https://doi.org/10.1007/s00167-009-1027-2.
- Zanguie, H., Sheikhhoseini, R., Yousefi, M. and Hides, J.A. (2024). Mechanical energy flow analysis in athletes with and without anterior cruciate ligament reconstruction during single-leg drop landing. Scientific Reports, [online] 14(1), p.1321. doi:https://doi.org/10.1038/s41598-024-51631-5.
- Disclaimer – The content here is designed for information & education purposes only and the content is not intended for medical advice.




