Clarifying the Role of Pain in Injuries
For a long time I dropped things, mostly smaller items like car keys. I also suffered from phantom pains. The tip of my finger itched even though it wasn’t there. – Tommy Caldwell, The Push

Image from www.quora.com
It wasn’t that far ago that phantom limb pain was a complete mystery. This is a sensation that someone experiences in, say their finger, after it’s been amputated. The finger no longer exists yet the person can still feel it. This is possible because sensations, such as pain, are experiences created by both your body AND your mind.
When a finger is amputated you lose the nerves that were part of the finger. You don’t lose the nerves that connect your finger to your brain, or the part of the brain dedicated to that finger. What remains are crucial components for the production of pain, and are sufficiently powerful to create pain in a limb that doesn’t exist. This is why phantom limb pain is possible.
This phenomenon has allowed us to learn a lot about how pain works. Unfortunately, misconceptions around pain are abundant, some of which dampen our ability to recover from injury. Clarifying the purpose of pain and how it works can go a long way in helping us overcome the most stubborn of injuries.
_ _ _
You’ve got a week left of training before you set-off for your fall climbing trip. You put your time in this year with the hopes of finally sending your long-time project. You’re feeling strong but will occasionally get an ache at the base of your left ring finger with hard bouldering sessions. It usually settles within a couple of days and you think nothing of it.
_ _ _
Pain is meant to protect you
When you experience pain, it is first and foremost a warning system meant to protect you from potential harm. If you take a finger and slowly start to pull back on it, you’ll experience pain before you cause tissue damage. This is meant to prevent you from going further so you don’t cause injury, and it happens in everyday life.
If you sit on a cold rock at the crag for too long your bum will get sore. This is meant to remind you to move around. You wouldn’t have caused harm to the tissue – it’s resilient! On the other hand, if you ignored the signal to move you may eventually sufficiently restrict blood flow to your bum and cause injury to the skin, known as pressure sores.
Perhaps a more pertinent example happens with training. If you’re pushing hard and nearing your body’s limits, you’ll start to get muscle soreness, mild pain, or straining in and around the joints. If you stop the session when the warning signs show up, there’s a good chance your tissues will settle within a few days and you’ll be good to start training again. The pains you experienced acted as a warning to tell you to back off so that your tissue can recover. Not heeding the warning is a good way to get injured.
_ _ _
This is your second day climbing and your third and final go at your project. It’s a gentle approach into a progressively crimpier pumpfest. It finishes with a deadpoint before locking-off to grab a jug. The terrain eases off significantly afterwards. Things are going well – your beta is clean and you’re moving quickly. Your left hand hits the edge of the deadpoint and you manage to curl your fingers into a full crimp. You pull into your lock-off and release your right hand. “POP” goes your left ring finger. You’re committed and finish the move. Only ten more feet of climbing. You think to yourself “that wasn’t painful” and finish the climb. As you lower you start to feel an ache in your finger. The next day, your finger is swollen, painful and difficult to move.
_ _ _
If you’re lucky, you’ll see an injury coming before it’s too late. We’re not all lucky and warnings don’t always present themselves. Pain is almost always associated with fresh injuries but when we experience the pain isn’t always consistent. Why are injuries painful, and why isn’t the timing of pain always consistent?

Photo Credit: Lauren Watson
A noxious stimulus sets off the alarm
In the example above, the “pop” was a sprain to the A2 pulley of your ring finger, a fairly typical climbing injury. You only start to feel an ache after you finish the route, though damage would have occurred with the pop instantaneously. Inflammation ensues. If there’s enough inflammation, nociceptors are triggered.
Nociceptors are nerve endings meant to detect a noxious stimulus. Once the nociceptor is triggered, it sends a signal up to the spinal cord. The spinal cord will then relay that message to the brain. If the brain determines that the nociceptive signal poses a threat, you will experience pain in your finger. By the time you come off the route, you’re starting to feel an ache and thinking “something is wrong”, all thanks to the inflammatory process that triggered your nociceptors.
Nociceptors can also be triggered by changes in temperature (e.g. a hot stove) and mechanical stresses (e.g. an aggressive stretch). The “pop” you felt would have triggered the mechanical nociceptors yet it wasn’t painful, an all too common occurrence. You were lucky enough to feel the ache immediately after completing the route. Some people won’t feel it until the next day, or in extreme examples, until they climb again a few days later. How can this be?
Nociception can be stopped at the spinal cord
The brain has a remarkable ability to lessen or even stop the noxious stimulus from making it all the way up to the brain. It can send a signal to the spinal cord that in essence says “we’ve got more important things to worry about (red-pointing this route!!), so don’t bother me with your nociception. I’m not interested right now.” This is why you don’t always feel pain with a very clear “pop”, and why climbers will often times finish a route before noticing their finger pain. This is also why you can run a marathon with a sprained ankle, and even win the race!
The brain listens to the danger signals
What happens when nociception makes it to the brain? The brain has the difficult job of interpreting all of the thousands of signals that come from the body at any given time. It needs to understand the signal before making a decision. Based on all of the information available to it, if it deems the signal to be dangerous to the tissue, and there aren’t more pressing matters, you will experience pain, whether it’s an ache, throb, sharp, lancinating, piercing, burning, stabbing, or (insert any pain descriptor) type of pain.
Now we know why we don’t always feel pain at the moment of injury, and we can explain the throb that occurs shortly after an injury. Let’s take a closer look at the alarm system as the healing process begins.
_ _ _
The rest of the trip was a bust. The finger progressively got worse. You could barely close your hand, making it impossible to climb. Thoughts about a long-haul recovery have taken over. It’s been two weeks since your injury and you find yourself sitting on your couch. You notice that the swelling and pain have finally started to settle. You decide to test it by lightly crimping your coffee table. BAM! “That *@#$ing hurt! This finger is totally messed.”
_ _ _
The alarm system sensitizes
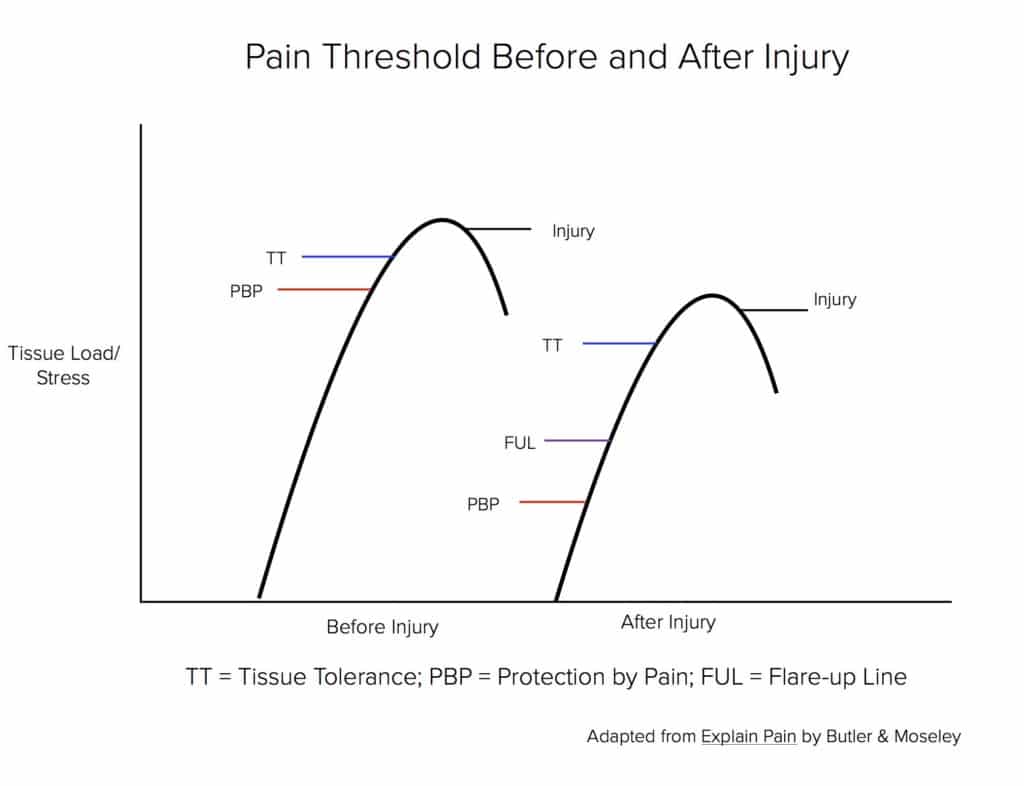
For simplicity’s sake, it’s easiest to think of two systems working together to help you recover from your recent injury. You have a system designed to heal your injured tissue and one to protect the tissue while it heals. Broadly speaking, the first consists of the inflammatory process, and the second creates your pain experience. Both are intricately connected and work together to get you back to health. While the inflammatory process repairs damaged tissue, the nervous system warns you against potentially harmful situations. Think of it as a smoke detector. If a sufficient amount of smoke is detected (nociception) it will sound the alarm (pain).
After an injury, your smoke detector is more sensitive. It will sound the alarm at the faintest hint of smoke, even if a fire (harm/ further injury) is far from a reality. This is your mind and body’s way of protecting the injured tissue so you don’t hinder or aggravate the healing process. You’ll experience pain far before you cause more harm. Remember that pain is meant to protect you.
During the coffee table incident, it’s far more likely that you triggered the alarm system without causing further harm. The pain typically settles relatively quickly without a significant increase in swelling, aching, or stiffness. Your warning system sounded the alarm to protect the already injured tissue.
The alarm system can be a helpful tool in the recovery process. It reminds you to drop into a lower gear and slow down. As the injury heals, and you begin to gradually load the tissues, the system will begin to desensitize and you’ll find yourself able to do more with less pain.
_ _ _
It’s been four weeks since the injury and the finger doesn’t seem to be improving much. The coffee table incident really freaked you out. It was quite sore for a few days afterwards. You went to grab a milk jug out of the fridge and even though it wasn’t as bad as the coffee table, you still felt pain. You wonder whether it needs more rest so you decide it’s best to avoid using the finger with other tasks – no milk jugs, no opening doors, light use with brushing your teeth and cutting food. Eight weeks out and it almost seems to be getting worse. Lifting a milk jug out of the fridge is more painful than it was three weeks ago. “What gives?!!” Four months out and lifting a milk jug out of the fridge is unthinkable. “Something must be seriously wrong.”
_ _ _
The alarm system can remain sensitized past healing
The experience of pain and the process of healing, though intricately connected, can diverge. It’s possible that as the healing subsides, the alarm system remains sensitive or even continues to sensitize. For instance, during the coffee table incident, your alarm system may have created a sufficiently noxious stimulus that you decided to avoid using the finger all together. Every time you use your finger your alarm system goes off and you go back to protecting the pulley that’s not healing. We often think that pain relates to tissue harm and that we should avoid anything that is painful. Remember that pain is meant to protect you and is a poor indicator of harm being done to your tissues.
If we continue to avoid using the finger in fear of causing harm, we may further sensitize our alarm system to the point that previously non-painful tasks become unthinkable. It’s possible that the healing process will finish and for the alarm system to remain sensitized. Rather than simply the pulley, your whole finger may become tender to touch. It may progress to your whole hand, forearm and upper arm weakening. This can be an incredibly frustrating, demoralizing, depressing, and for some a life altering experience. The good news is that the human body is adaptable no matter your age, and pain is changeable, no matter how long you’ve had it or the severity of your injury.
Desensitizing the Alarm
A sensitized alarm system needs desensitization, and one of the best ways of doing this is by understanding how pain works. We now know that pain is meant to protect you. We also know that pain is a poor indicator of tissue harm, and can occur even when no harm is being done to your tissue. We also know that pain can persist past healing.
Armed with this knowledge the next logical step is to say “Hell! If my alarm is overactive I may as well ignore and push through the pain”. False! This can be a good way of making the situation worse. Remember that you may have avoided exposing your tissue to stresses such as lifting a jug of milk. Not only does your nervous system need desensitization, your tissues need to adapt to the load you’re exposing it to. In other words it may need some time to adapt to lifting a milk jug again. When re-introducing movement and activity, I typically have my clients ask themselves two questions:
1. Is this safe for me to be doing?
To phrase it differently, am I exposing my tissues to a safe load? When I lift the jug of milk out of the fridge, I may experience a bit of pain, but can my tissues handle this load? Remember that pain is not an indicator of tissue harm, and with a sensitized system you’ll experience pain before you cause harm. If you don’t know the answer to this question it’s best to start more conservatively. Can my finger handle holding a phone despite some pain? Chances are yes, but for some this might still be too much to start with. Can I bend my finger despite mild pain? Lightly moving your finger through its available range of motion is typically a very safe bet if you have any doubt. The next thing I ask is:
2. Will I be OK tomorrow?
There are a lot of reasons for why pain may not always present itself immediately after a stressor. This is why it’s important to ask yourself whether you’ll feel pain later. Take comfort in knowing that pain that lasts a couple of days, though irritating and perhaps demoralizing, is unlikely to cause any more harm to the injured tissue. We refer to these as flare-ups of the nervous system, and are perhaps not surprisingly relatively common. This is normal, and provides an opportunity for evaluating how hard you’re pushing. When a flare-up happens we typically need to pull back to rest the nervous system. Once the pain has calmed down we then try a similar activity at a lesser intensity. The idea is to build your activity levels gradually and systematically.
In his book The Push, Tommy Caldwell describes exactly this process when he was overcoming a sensitized finger stump and experiencing phantom limb pain. Although an extreme example, the process is the same. He gradually and systematically exposed his new finger to more aggressive exercises and tasks to the point of climbing the Dawn Wall.
Overtime you’ll find yourself using your finger with everyday tasks, lightly crimping coffee tables, and even starting to try easy rock climbs. Eventually you’ll start bearing down on crimps and building the confidence to try your old projects. Gradually building your tolerance to movement and activity, while simultaneously pacing your activities to avoid delayed pain are great tools in helping you overcome a sensitized alarm. If you need help getting there, look for a physical therapist well versed in the latest pain science and exercise physiology. If we stick to the finger, the end-stage rehab usually consists of fingerboarding. If your therapist is recommending more soft tissue work three months post injury, it’s time to look for someone else. Remember that gradual loading and pacing is your best bet no matter the injury.

_ _ _
It’s been a year since your finger injury and you find yourself looking at the old project that started it all. You strap on your shoes, tie into your harness and begin making your way up the gentle approach leading to the crux. You can feel your heart pumping in your chest. The nerves are mounting. You take a few deep breaths before starting the long and pumpy crux. The finger feels great – not an inkling of pain or discomfort. You hit the deadpoint with the left hand, curl your fingers into a crimp, release the right hand and reach for the jug leading to easy terrain. You don’t even feel pumped as you’re lowered to the ground.
_ _ _
Is it possible to come out stronger than you started? It sure as hell is.
Written By William Bateman

William Bateman owns and operates ProjectPhysio.com, a clinic and website designed to help his clients recover from injury, prevent injury, and overcome performance plateaus. Will’s practice is guided by two principles: he uses science and evidence to help guide treatment decisions, and believes that knowledge is power – the more you know, the better your outcome. He places an emphasis on active recovery, self-directed pain management strategies, pain neuroscience, and graded exercise programs to help his clients reach their goals.
Will is responsible for developing and managing the Ground Up Performance Team, bringing together healthcare providers, climbing coaches, strength and conditioning specialists, and exercise physiologists to provide climbers with sport-specific services. His team is constantly re-evaluating the best tools for measuring performance and preventing injury in climbers. He currently oversees athlete monitoring and injury prevention for the Ground Up Youth Competitive Climbing Team and the Quest University Climbing Team. Will has developed numerous injury prevention programs for climbers, skiers, snowboarders, runners, and swimmers, and has spoken about the topic throughout Canada and the USA. He also runs chronic pain education workshops to help demystify the complexities of pain.
Will is a mentor with the Canadian Physiotherapy Association – Pain Science Division for clinicians looking to learn the latest in pain neurophysiology and its application to rehabilitative sciences.
Edited by Nina Tappin

Nina Tappin has been treating sports injuries since she graduated as a physiotherapist from McGill University in Montreal, Canada in 1999. She has a wealth of experience in treating rock climbers, university athletes, and general orthopedic cases.
Nina is a member of the U.K. ACPSEM (Association of Chartered Physiotherapists in Sport & Exercise Medicine) and has her Silver level of accreditation. She has been mentored by some of the top physiotherapists in sport in the U.K..
Nina has been a dedicated rock climber since 2000, and has been treating rock climbing related injuries ever since. She has treated some of Britain’s elite rock climbers, such as, Hazel Findlay, Ben West, Neil Gresham, Tim Emmett, and Charlie Woodburn. Nina has also treated members of the GB lead climbing, and bouldering junior and senior teams. She treats novice and intermediate level climbers on a regular basis.
Nina writes articles in Rock & Ice, CLIMB magazine and on UKC website. She also teaches “Common Climbing Injuries & Injury Prevention” Modules to climbers and instructors at various climbing walls, and on Neil Gresham’s Masterclass Academy Coaching Course.
Nina has a special interest in injury prevention amongst children and females in sport. She is also interested in advising women who are pregnant, and/or recovering from birth on how to exercise, and climb safely.
To Learn More Visit:
- Disclaimer – The content here is designed for information & education purposes only and the content is not intended for medical advice.





awesome article!
Wow this is great! So relevant and something not talked enough about in climbing. When you look up “fear of injury in climbing” you get mostly tips to address falling but “fear of injury in sports” is a much richer search, with sports psychology, case studies, and mental training, etc. This article is definitely bringing our understanding closer to the latter.